San Diego Orthodontics
San Diego Orthodontics
Orthodontics
Orthodontics
Occlusal Change Through Orthodontics in TMD Patients
October 1, 2007 | See the original article in Dentistry Today.
Although some claim that occlusion has little effect on a healthy TMJ and is not generally a causal factor in TMD, many have made emphatic claims to the contrary. Many orthodontic practices are positioned in the marketplace as providing proven treatment for TMD, yet some patients seem to experience TMD as a consequence of orthodontic treatment.
While existing literature reports that orthodontics can both help and worsen TMD, this paper describes two cases where TMD relief was successfully achieved through orthodontic therapy. More specifically, these cases lend credence to the theory that increasing the vertical dimension and removing retrusive forces on the mandible may help recapture the disc that can be displaced by over-closure of the mandible.
Case 1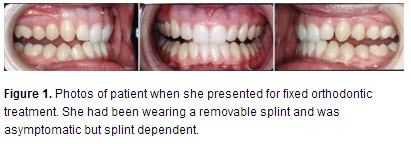
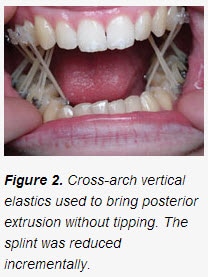
Case 1 describes treatment that utilized a hard acrylic, flat-planed splint to alleviate TMD symptoms of pain, popping, and clicking by advancing the mandible and increasing vertical dimension. The patient was “splint dependent” but symptom-free at the stage she was transferred for orthodontic treatment (figure 1). The pain returned whenever she was not wearing her splint for consecutive days because she returned to an “over-closed” position. Once orthodontic treatment commenced, the splint was reduced incrementally, allowing teeth to supra-erupt. This was done sequentially until the natural occlusion mimicked the patient’s occlusion with the splint. It was reduced from the posterior forward, allowing the second molars to supra-erupt in a controlled fashion. It was also sequentially reduced in thickness. Mobility from the orthodontics facilitated this occlusal setting. Three distinct aspects of the patient’s occlusion were changed, which helped provide TMD relief:
- The maxillary incisors were flared labially with treatment. Lingually inclined lower incisors translate occlusal force into a retrusive direction as the patient closes, especially during protrusion. This was eliminated as labially upper and lower incisors deliver chewing force in a more vertical direction into the alveolar bone, decreasing the tendency of the mandible to be pushed backward and minimizing disc trauma.
- Similarly, the incisors had greater vertical overlap initially. This compounded the problem caused by the retroclined position, as the entire facial surface of the lower incisors was acting as a receiving surface for “pounding” by the maxillary incisors. The posterior definition better tolerates this vertical chewing force.
- The molar extrusion and improved interdigitation, in conjunction with occlusal adjustment, provided a more stable posterior occlusion. This offers better protection against retrusive slides in centric and during mastication, which can further exacerbate TMD.
 Bands Molar extrusion achieved using cross-arch elastics (Figure 2) from the buccal of the upper teeth to the lingual of the lowers as well as lingual of the upper teeth to the buccal of the lowers served to extrude the posteriors with greater control and no buccal-lingual tipping.
Bands Molar extrusion achieved using cross-arch elastics (Figure 2) from the buccal of the upper teeth to the lingual of the lowers as well as lingual of the upper teeth to the buccal of the lowers served to extrude the posteriors with greater control and no buccal-lingual tipping.
Although the causal factors of TMD are often a mystery, this case demonstrates that eliminating obvious and severe occlusal abnormalities through splint therapy and gradually through orthodontics, may provide TMD relief and minimize occlusal wear as the traumatic occlusion is eliminated (Figure 3).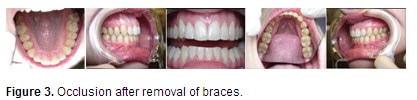
Two years after treatment, the patient was orthodontically stable and symptom-free.
Case 2: Bilateral TMJ
The second case shows a patient who had bilateral TMJ clicking and tinnitus. He had second molar occlusion only, a constricted maxillary arch, occlusal trauma, and wear (Figure 4).
The patient wore posterior cross-arch elastics from the lingual of the maxillary posterior to the buccal of the mandibular posteriors to achieve proper intercuspation, and bilateral, evenly distributed tooth contacts, as a posterior cross-bite has been associated with TMD. The upper posteriors were stabilized with a Hawley retainer. The upper and lower anteriors were stabilized with lingual Ribbond splints (Ribbond) canine to canine.
This effectively stabilized rotated teeth (in conjunction with fiberotomy) and provided proper resistance form to the restored incisal composites, necessary because of the previous occlusal trauma (Figures 5 and 6).
The incisal edges became much more durable once connected to the splint because of increased thickness.
The TMJ, occlusion, and restored incisal surfaces were all stable at recall (Figure 7).
Conclusion
While TMD is often a mystery and is even seen in many normal occlusions, frequently other factors exist, such as a history of trauma, bruxism, or degenerative joint disease of a systematic nature. However, these two cases show at least one obvious and proximate cause for their TMD, which is an unstable occlusion.
Acute inflammation can be mitigated through ice, NSAIDS, and splint therapy until subsequent inevitable exacerbations occur. Definitive treatment through permanent occlusal change sometimes is the only hope for these patients, and is still not a panacea if disc damage has occurred or if occlusal abnormalities are not corrected.
While all aspects of orthodontic TMD treatment have not been substantiated in the literature, providing the patient with a stable, evenly distributed occlusion with correct buccal-lingual molar and nonretrusive incisor relationship, as well as providing an increased vertical dimension, may be a good place to focus in treating this elusive problem.
Make an Appointment
Visit our San Diego cosmetic dentistry and family dentist office, conveniently located at University Town Center in La Jolla. Call (858) 552-1223 to schedule your consultation with Dr. George today.