TMJ Treatment San Diego
Dr. George is a true healer. I came into his office with little hope due to some intolerable pain in the ear/neck/jaw. Was suffering from a severe flare up from TMJ due to being in a chair for too long from my previous dentist. Dr. George was thorough in his evaluation. I left his office with solutions. In my case some Botox and a cortisone shot to my left joint in the jaw. I instantly felt the release and it took the edge off. He kindly recommended a chiropractor and called them to make some room for me. Just FANTASTIC! One of the best days I have felt in two months. There is hope. There are good people out there. This dentist is one of them. Wonderful and highly recommended from someone who was starting to lose themselves in pain. Plus he saved me from getting 9 fillings that my previous dentist said I needed but It ended up not being the case.
TMJ Treatment in San Diego
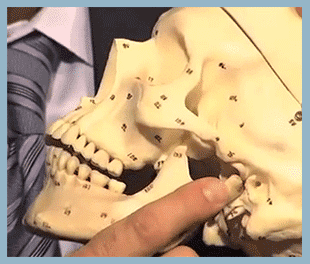
As a TMJ dentist, Dr. George is here to offer the best TMJ treatment in San Diego. Many people who suffer from TMD or TMJ don’t know that there are safe and easy ways to eliminate jaw pain. Often caused by misaligned joints, jaw pain can negatively affect your life and stop you from participating in simple daily activities. Dr. George can assess your symptoms and determine whether your jaw pain may be related to temporomandibular joint disorder, called TMJ or TMD for short. TMJ syndrome is a term that covers acute or chronic inflammation of the temporomandibular joint. In many cases, TMJ Disorder is the result of physical damage to the joints. For example, the soft cushioning discs may be out of place. It can also result from inflammation in the nearby muscles and ligaments.
If you you clench or grind at night or during the day, this habit could be the root of your jaw pain. Other times, injury, malocclusion, or heredity cause jaw pain. Stress is also a very common factor.
If you believe you may be suffering from jaw pain caused by misaligned joints, it is important to seek treatment right away. Untreated TMJ syndrome can lead to more severe issues such as bruxism, dental erosion, malnutrition, hearing loss, and permanent jaw damage.
Relief from jaw pain may be as simple as wearing a custom-made oral splint that relieves pressure in the jaw joints. If you’re looking for the best TMJ or TMD treatment, Dr. George is the dentist for you.
Stay connected, like us on Facebook!

TMJ Symptoms
Symptoms of TMJ may include jaw pain, tenderness or clicking sounds when opening and closing the mouth, difficulty chewing, headaches, and earaches. Proper diagnosis and treatment can help alleviate these symptoms and restore proper joint function. If you experience any of these symptoms, it’s important to see a dentist or doctor as soon as possible for proper evaluation and treatment.
- Tinnitus
- Migraines
- Chronic Headaches
- Ear pain/ringing in the ears
- Neck/Eye Pain
Make an Appointment
Visit our San Diego cosmetic dentistry and family dentistry office, conveniently located at University Town Center in La Jolla. Call (858) 552-1223 to schedule your consultation with Dr. George today.